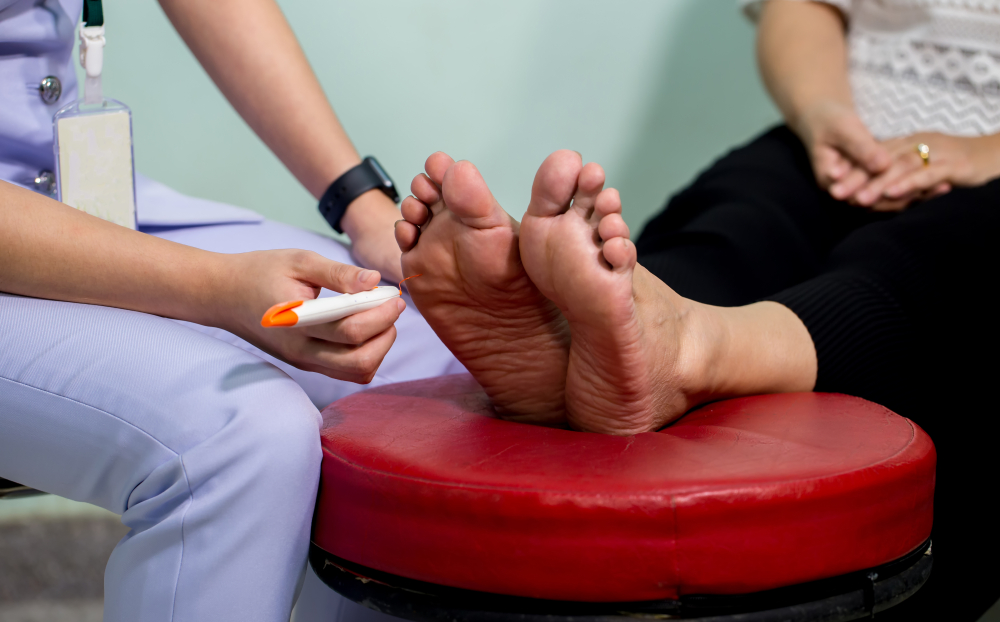
Diabetes mellitus poses significant dangers to health, including blindness, hypertension, and cardiovascular diseases. However, diabetic foot, responsible for 50% of non-traumatic lower-limb amputations, is often overlooked.
Understanding why diabetic foot complications occur is essential.
Peripheral neuropathy: A loss in sensing danger
High blood sugar damages nerves in legs and feet over time, a condition called peripheral neuropathy.
This leads to plantar dryness and foot deformities. The loss of sensation prevents recognition of injuries, delaying treatment for diabetic foot.
Damage to the nervous system is particularly dangerous when combined with circulatory issues.
Warning signs of peripheral neuropathy include:
- Tingling in feet and legs;
- Progressive numbness;
- Reduced sensitivity to temperature changes.
Vascular disorders linked to diabetes
High blood sugar causes circulatory problems such as:
- Arteriosclerosis: hardening and decreased elasticity of arteries supplying feet and legs;
- Hypertension: excessive blood pressure burdening the heart;
- Atherosclerosis: accumulation of fatty deposits in the arteries.
These disorders disrupt blood flow, hinder healing, and make diabetic feet more vulnerable to damage.
Watch for recurring symptoms such as:
- Bruising;
- Open wounds;
- Nodules (blisters);
- Accumulated corns or calluses;
- Cracks and splits in feet or heels;
- Swelling;
- Redness.
Consult a doctor immediately if an injury is detected on a diabetic foot.
Consequences of lack of treatment
Peripheral neuropathy and vascular disorders make early treatment of diabetic foot lesions vital.
Without treatment, reduced sensation and impaired healing can lead to amputation.
The progression towards amputation usually involves:
- Infection;
- Development of ulcers;
- Necrosis (gangrene) of infected tissue.
Amputation aims to remove necrotic tissue and stop ulcer spread.
Preventive treatments for diabetic feet
Amputation is a last resort. Before that, several podiatric treatments can preserve foot health.
Common treatments include:
- Foot orthoses to correct foot shape changes;
- Relief shoes to protect and prevent wound reopening;
- Custom orthopedic shoes to reduce pressure on deformities;
- Foot care involving moisturizing, nail maintenance, and preventive exams.
Consult a podiatrist before amputation becomes necessary
Regular consultations with a podiatrist are essential for people with diabetes.
Podiatrists can detect lesions early to prevent infection and amputation.
Contact your PiedRéseau clinic for diabetic foot care and symptom treatment.